Digitally Engineering
Tomorrow, Today
Building future-ready enterprises through innovation and
strategic partnerships
Quality Certifications
Infinite Re-Appraised at CMMI V2.0 Maturity Level 5 for Development and Services
Know More
Corporate Sponsorships
Proud Sponsors of Major League Cricket's Washington Freedom
Know More
Partnerships
Infinite Partners with ServiceNow to Deliver Personalized, Automated and Intuitive Client Experiences
Know More
Industry Focus
Delivering next-gen digital experiences across industries

Healthcare
Seamlessly delivering end-to-end digital health experiences

Banking, Financial Services & Insurance
Driving transformation with our banking, financial services, insurance, and payments experts


High Technology
Solving real world challenges through rapid innovation and cutting-edge R&D

Media & Entertainment
Bringing our clients secure, seamless, and advanced enterprise messaging

Government
Modernizing IT for digital-first experiences for state, local, and federal agencies


Future Ready Services
Transforming enterprises with innovative digital solutions
Delivering value for our customers
Digitally Engineering Tomorrow, Today
Foster a Digital Workforce
At Infinite our employees have the opportunity to advance their careers while solving customer challenges using the latest digital technologies


Executive
Leading Administrator Health Benefits Plans
CIO Fortune 500
Warranty Insurance Provider
CIO
Financial Institution
CTO
Insurance Industry

Our Offices
Our Offices
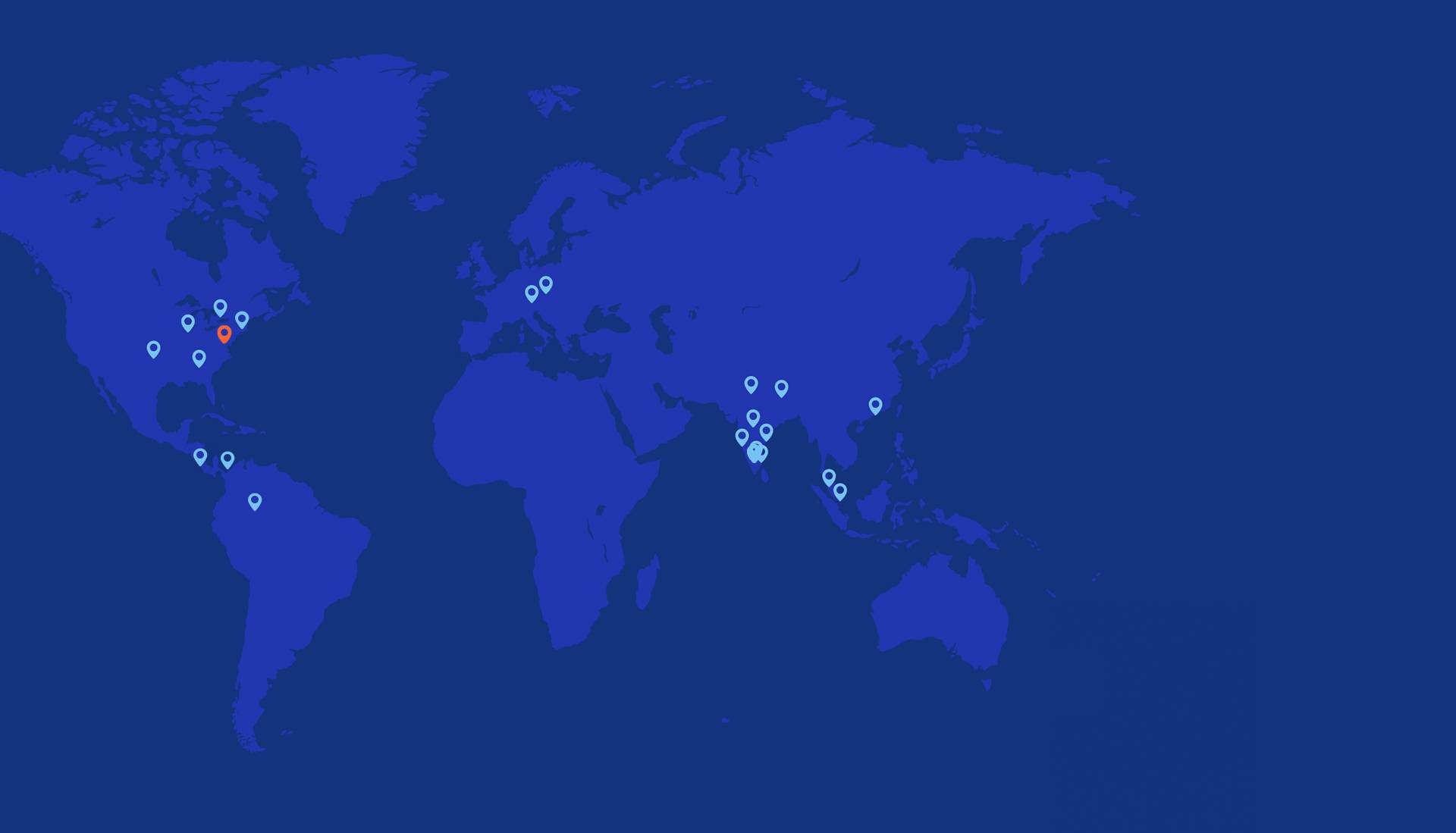
Heredia, Costa Rica
Metro Free Zone,
Barreal de Heredia,
CR 40104
MacArthur Boulevard,
Irving, TX 75038
3219 & 3231, N Wilke Road,
Arlington Heights,
IL 60004
1801-1 Yonge St,
#99 Toronto,
ON M5E 1W7
• Headquarters
2600 Tower Oaks
Blvd Suite 700, Rockville,
MD 20852
11800 Amber Park Dr,
Alpharetta,
GA 30004
Viktualienmarkt 8,
München,
DE 80331
Revolucni 7 Prague,
CZ 11000
Hong Kong
Unit A-1-15, Coplace
2,2260 Jalan Usahawan 1,
MY 63000
20, Changi South Avenue 2,
SG 486547
Unit 5 & 6,
Phoenix Fountainhead,
Tower 3,
MH 411014
Plot No. 1, Hill # 3,
APIIC IT / ITES SEZ,
Rushikonda,
Madhurawada,
AP 530045
Unit 45/46, Block 3 SDF Buildings,
MEPZ Tambaram, TN 600045
TVH Agnitio Park, 2nd Floor,
Old Mahabalipuram Road, TN 600096
1st Floor, Gamma Block Alpha City Complex 25,
TN 600110
Gurugram
Plot No. - 21,
Institutional Area Sector- 44,
HR 122001
New Delhi
155 Somdutt Chambers-II 9
Bhikaji Cama Place,
DL 110066
Noida
A-94/9, Sector 58,
Gautam Buddha Nagar,
UP 201301
157, EPIP Zone, Phase 2,
Kundalahalli, Whitefield, KA 560066
GEIPL-SEZ, Global Axis,
Block 2(A1), EPIP, Whitefield, KA 560066
Module No 1,
Q3-A1 & A3 Quadrant 3,
1st Floor Cyber Towers, AP 500081
#5, Plot No-24, Raj Enclave,
Sai Lok, GMS Road, Dehradun,
IN-UT 248001
36 Crosby Drive Bedford,
MA 01730
Panama City, Panama
Bogota, Columbia
Hattisar Sadak 429,
Ward No. 1, Kathmandu,
Nepal – 44600
North America
• Maryland, USA – Headquarters
Atlanta, USA
Chicago, USA
Irving, USA
Boston, USA
Toronto, CA
Central America
Heredia, Costa Rica
Panama City, Panama
South America
Bogota, Columbia
Europe
Munich, DE
Prague, CZ
India – South Asia
Bengaluru, IN
Chennai, IN
Dehradun, IN
Gurugram, IN
Hyderabad, IN
New Delhi, IN
Noida, IN
Pune, IN
Visakhapatnam, IN
Southeast Asia
Hong Kong
Malaysia
Singapore
South Asia
Nepal












